Unlike other children his age, Kai (not his real name) spent little time playing with other children. Sometimes he would inform his mother that he had no pals at school.
“I have been referred to as ‘fatty’ and ‘chubby’ by peers. It made me feel different from them, therefore I rarely interacted with or played with them,” he explained.
Kai is 1.62m in height and 70kg in weight. This results in a body mass index (BMI) of 26,7, which places him at a moderate risk for obesity-related disorders. His BMI exceeds the 95th percentile for his age group.
Singapore’s obesity rates are increasing, particularly among children and teenagers. The percentage of elementary, secondary, and pre-university pupils under the age of 18 who were overweight increased from 13% in 2017 to 16% in 2021.
According to the Ministry of Health, the majority of the rise occurred during the last two years of the COVID-19 pandemic (MOH).
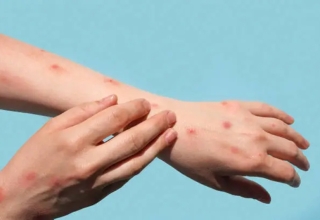
However, myths regarding obesity persist, resulting in fat-shaming attitudes and an excessive focus on the number on the scale. Both can negatively impact the health of youngsters, physicians told CNA.
Due to his stature, Kai has been taunted, bullied, and discriminated against, according to his mother, who requested that neither she nor her son’s identities be used.
She decided to bring him to a general practitioner after observing that he appeared to be larger than his contemporaries. She was scared that Kai might lose confidence or give up if his weight problem worsened.
Kai began therapy at the weight management clinic at KK Women’s and Children’s Hospital (KKH) approximately six months ago. The facility is staffed by a paediatrician, fitness specialists, dietitians, psychologists, and medical social workers.
The modifications were immediate. His mother stated that the first thing to go was the fast food that Kai used to consume “quite frequently.”
Because Kai’s mother worked as a software engineer, his grandmother was his primary caregiver. They made adjustments after realizing that Kai could be taking up poor eating habits from the grownups.
The family now eats three meals each day, consisting primarily of rice with meat and veggies and bread. They spend approximately $300 per week on groceries.
The way in which Kai used his free time also changed. As did many children of his age, he enjoyed playing mobile and computer games. He did not like to workout.
Keep Reading
After KKH devised an organized fitness program for him, he became more physically active, swimming, playing team sports, and taking weekend nature walks.
Over time, the changes become inwardly focused. His mother stated that while working with his pediatrician, Kai became more self-assured and began taking responsibility for his weight management.
The doctor in paediatric endocrinology stated that what important is instilling healthy habits that the child maintains on their own, long after any external weight management program has ended.
This also contradicts a common theme he hears from parents of overweight boys, namely that National Service (NS) would solve the problem if no action is taken sooner.
Dr. Sng stated that by the time their sons lose weight during National Service, it may be too late to modify their attitudes toward fitness. He cautioned that they could gain the weight back after leaving the regimented environment of the military.
Insufficient consumption of fruits and vegetables and excessive consumption of carbohydrates and fats are the leading causes of obesity.
Dr. Elaine Chew, head and senior consultant of the Adolescent Medicine Service at KKH, stated that insufficient physical activity and an increased reliance on automobiles as opposed to walking also add to the problem.
Inadequate sleep and excessive use of computers, mobile phones, and television are all problems, she added.
However, some things are beyond an individual’s control. Dr. Chew stated that genetic and cultural variables, such as a family history of obesity, can also contribute.
And as Kai’s situation demonstrates, the risk of obesity is also affected by the availability of resources such as money and time, as well as their effect on food intake.
Kai’s mother stated, “Healthy food typically requires more time to prepare, but unhealthy food such as fast meals and snacks like potato chips are much more accessible and may even be cheaper.”
Dr. Sng referred to this as the poverty-obesity paradox, in which food insecurity is paradoxically connected with a greater risk of obesity.
Researchers hypothesize that this is due to the high-calorie, appetizing meals consumed by individuals with inadequate food security, as well as the lack of knowledge, time, and resources required to engage in healthy eating and activity.
The National Population Health Survey 2020 conducted by the Department of Health appears to reflect this. As a proxy for socioeconomic characteristics, the poll uses the greatest level of education achieved.
16.3% of adults with an elementary education or less had the greatest prevalence of obesity. The percentage decreased to 12.5% for those with secondary education and 8.9% for those with post-secondary education.